
The Economics of the Fortress: Breaking Institutional Friction in Nursing
Author: Jude Chartier RN / AI Nurse Hub Date: March 30, 2026
By: Jude Chartier RN / AI Nurse Hub
Date: March 4, 2026
Introduction
The American home care industry faces a dual crisis: a massive labor shortage and a systemic failure to provide safe, affordable, and consistent care. While the current paradigm prioritizes “human-centric” care, this model is increasingly defined by high turnover, caregiver burnout, and significant risks of elder abuse and financial exploitation. This article examines the transition toward embodied humanoid robots as a superior alternative for task-oriented home care. By analyzing the Return on Investment (ROI) for care providers, the diagnostic advantages of continuous AI monitoring, and the ethical safeguards of unbiased mechanical care, this paper argues for a nurse-led hybrid model. In this model, humanoid robots perform high-risk and repetitive labor, while Registered Nurses (RNs) utilize real-time data to exercise complex clinical judgment, effectively elevating the standard of care for an aging population.
I. Introduction: The Systemic Vacuum in Home Care
In early 2026, the venture capital sector signaled a profound shift in healthcare priorities, with cumulative investment in humanoid robotics reaching record highs. This influx of capital occurs against a backdrop of domestic labor stagnation; home health aides (HHAs) remain among the lowest-paid workers in the United States, often earning wages that barely clear the federal poverty line (PHI, 2024). This economic disparity has created a “vacuum of care” where the demand for services—driven by the fact that one in five Americans will be over 65 by 2030—far outstrips the available human workforce.
The prevailing discourse often critiques the “robotic solution” as a cold replacement for human empathy. However, this sentimentality ignores the structural failures of the current system. For the healthcare entrepreneur and the clinical nurse leader, the move toward automation is not merely an act of cost-cutting; it is a proactive strategy to stabilize a volatile industry, mitigate liability, and provide a level of clinical vigilance that human labor, by its biological nature, cannot sustain.
II. The Financial Architecture of Care: Displacing the Human Capital Trap
For home care agency owners, the primary barrier to profitability and service continuity is the “churn” of human capital. The current agency model—billing $35 per hour while paying a worker $16—is often unsustainable due to the “direct care labor trap,” where administrative costs consume the margin.
1. The Financial Burden of Attrition
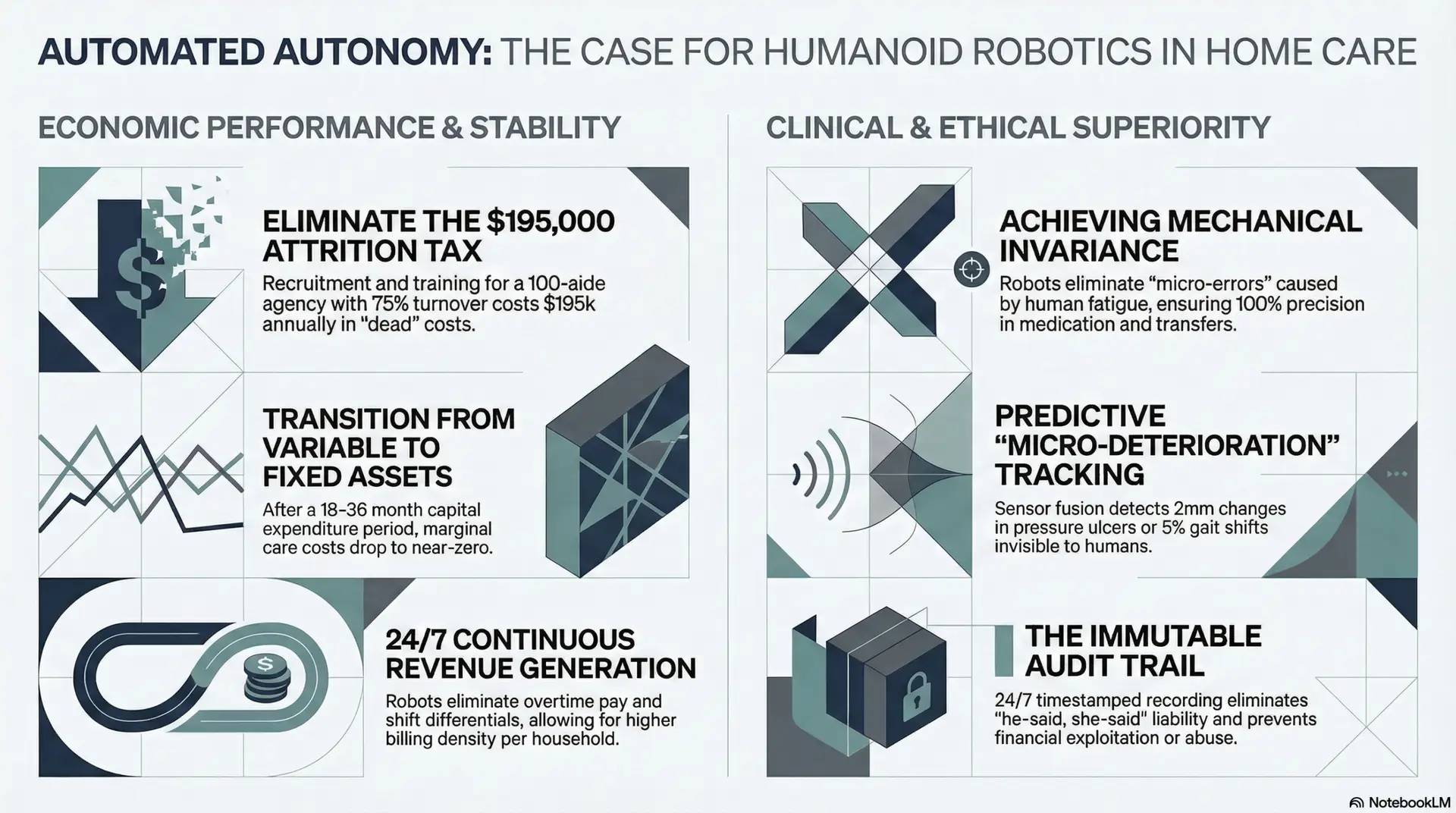
The home care industry experiences an annual turnover rate ranging from 75% to 100%. According to updated data from Activated Insights (2025), the cost to recruit, onboard, and train a single replacement caregiver is approximately $2,600. In a mid-sized agency employing 100 aides, a 75% turnover rate results in an annual loss of $195,000. These are “dead” costs that provide zero value to the patient.
Furthermore, the “ghost costs” of human labor—including payroll taxes, workers’ compensation, and the administrative overhead of scheduling 24/7 coverage—often reduce an agency’s net margin to less than 5%. Humanoid robots represent a fixed asset. Once the initial Capital Expenditure (CapEx) is cleared—a period typically spanning 18 to 36 months depending on utilization—the marginal cost per hour of care drops to near-zero, covering only electricity and periodic software maintenance.
2. Elimination of Administrative Overhead and “Ghost” Costs
Human labor requires a massive backend infrastructure. Schedulers must manage personal emergencies, sick leave, and interpersonal friction between staff and families. A robotic workforce eliminates these operational bottlenecks. Robots do not require scheduling adjustments for childcare issues, they do not file for unemployment, and they do not require the constant HR oversight necessitated by human temperament. For the business owner, this allows for a “lean” agency model where revenue is directed toward clinical innovation rather than administrative firefighting.
III. The Comparative Economic Advantage: Why the Robot Model Wins
The transition to a robotic model provides a decisive ROI by transforming care from a variable-cost service into a predictable, high-margin asset.
1. Liability Reduction and Insurance Premiums
Human-led care is a high-risk insurance environment. Professional liability and workers’ compensation premiums are driven by caregiver injuries and patient incidents. Humanoid robots, equipped with high-torque actuators and multi-axis balance algorithms, are physically superior for high-mass labor. By eliminating “human failure” in transfers, agencies can negotiate significantly lower insurance premiums. Furthermore, the “audit trail” provided by a robot’s 24/7 recording capabilities effectively eliminates the “he-said, she-said” liability in abuse or theft allegations, protecting the agency from catastrophic legal settlements that can bankrupt a startup.
2. 24/7 Revenue Generation and Scalability
A human aide is limited by labor laws, overtime protections, and the biological need for rest. A humanoid robot provides 24/7 presence without the compounding cost of time-and-a-half or shift differentials. For families, this provides “all-in” security for a flat monthly fee; for the agency owner, it creates a continuous revenue stream that is not capped by the number of hours a human is physically capable of working. This 24/7 capability allows for a higher “billing density” per household, dramatically improving the lifetime value (LTV) of each client.
IV. The Mechanical Advantage: Surpassing Biological Limitations
The classification of home care as “unskilled” labor is a profound mischaracterization. However, when evaluating the delivery of care, the robotic model demonstrates a clear superiority in terms of consistency and diagnostic accuracy.
1. Precision vs. Biological Variability and “Mechanical Invariance”
The human caregiver is subject to “biological variability”—fluctuations in performance dictated by fatigue, mood, and stress. An embodied humanoid robot operates with “mechanical invariance.” Whether it is the first or the twenty-fourth hour of a shift, a robot performs a transfer or a medication administration with the exact same level of precision. Human aides, particularly those working double shifts to overcome poverty-level wages, are prone to “micro-errors” such as skipping a skin check or mismeasuring a dose. These errors cumulatively degrade patient health and increase agency liability.
2. AI-Enhanced Clinical Vigilance and “Micro-Deterioration” Tracking
A humanoid robot provides continuous, data-driven diagnostic monitoring that no human can match. Utilizing sensor fusion (Lidar, Computer Vision, and thermal imaging), robots can detect “micro-deteriorations” invisible to the human eye. A robot can identify a 2-millimeter change in a pressure ulcer or a subtle 5% change in gait symmetry that indicates an impending stroke or neurological event (Grand View Research, 2025). This allows the agency to pivot from reactive care to predictive care, significantly reducing hospital readmissions—a key metric for Medicare reimbursement and agency reputation.
V. The Ethical Imperative: Eliminating Abuse and Exploitation
The safety of the patient is the most provocative advantage of the robotic model.
1. Mitigation of Elder Abuse and Compassion Fatigue
KFF (2025) indicates that 1 in 10 older adults experience mistreatment. Human caregivers are susceptible to “compassion fatigue,” where emotional exhaustion leads to irritability or neglect. A robot is incapable of anger. It provides a standardized, patient-centered response regardless of the patient’s behavior, ensuring that dementia-related aggression is met with de-escalation rather than retaliation. This creates a psychological “safety floor” for the patient and a “liability floor” for the agency owner.
2. Financial Integrity and Auditable Care
Theft of medications, jewelry, or identity is a significant liability in the domestic care market. Humanoid robots provide a persistent, immutable audit trail. Every interaction is timestamped and recorded, creating a transparent environment that protects the patient’s assets. For the business owner, this transparency is a powerful marketing differentiator, offering peace of mind that human agencies simply cannot guarantee.
VI. The Nurse-Led Hybrid Model: Elevating Professional Practice
In this model, the Registered Nurse (RN) assumes the role of a “Clinical Data Overseer.” By delegating repetitive physical labor to humanoid robots, the nurse is freed to work at the “top of their license.” The robot serves as the nurse’s remote surrogate, allowing the RN to:
VII. Conclusion: Embracing the Future of Reliable Care
The home care industry is being rescued by robotics. For nurses and entrepreneurs, the ROI is clear: lower turnover, reduced liability, and a level of clinical monitoring that human labor can never achieve. We must move past the guilt of automation and embrace a future where care is defined by its reliability, not just its pulse. By transforming the “dirty, dull, and dangerous” tasks of home care into an automated, data-driven process, we empower clinicians and protect the most vulnerable members of our society.
References
Activated Insights. (2025). Benchmarking Report on Caregiver Turnover and Recruitment Costs. Retrieved from [Industry database].
Grand View Research. (2025). Elder Care Assistive Robots Market Size, Share & Trends Analysis Report, 2025-2033.
KFF. (2025). Staffing Shortages and Deficiency Trends in Long-Term Care Facilities. Kaiser Family Foundation Research Series.
PHI. (2024). The State of the Direct Care Workforce: 2024 Data and Trends. Policy Research Report.

Author: Jude Chartier RN / AI Nurse Hub Date: March 30, 2026

By: Jude Chartier RN / AI Nurse Hub Date: March 23, 2026

By: Jude Chartier RN / AI Nurse Hub Date: March 19, 2026