
The Economics of the Fortress: Breaking Institutional Friction in Nursing
Author: Jude Chartier RN / AI Nurse Hub Date: March 30, 2026
Author: Jude Chartier RN / AI Nurse Hub
Date: March 17, 2026
Abstract
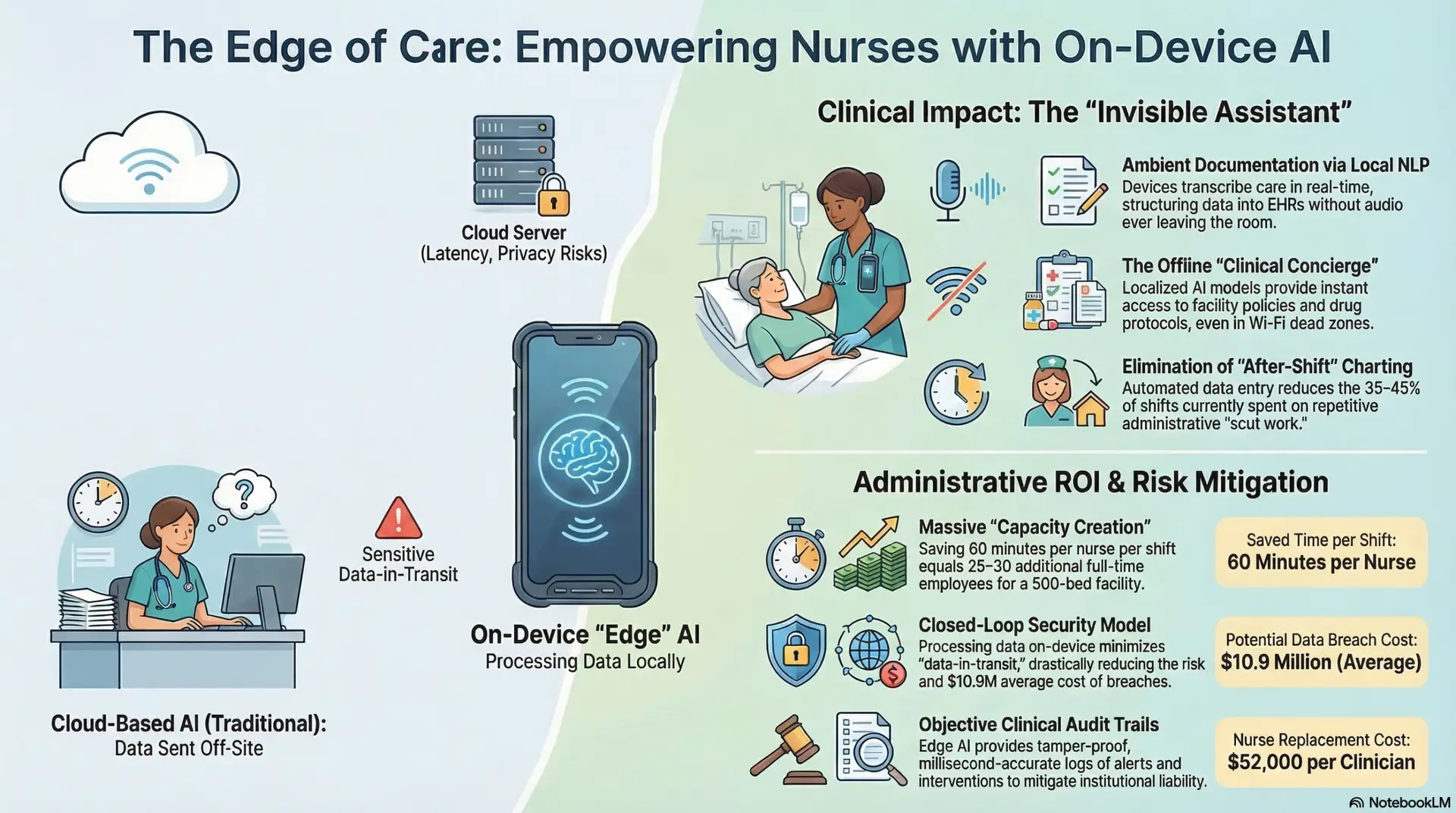
As healthcare institutions face unprecedented levels of nurse burnout, compassion fatigue, and acute staffing shortages, the integration of Artificial Intelligence (AI) has shifted from a luxury to a primary strategy for operational recovery and clinical support. However, traditional “cloud-based” AI—which relies on off-site data centers—often introduces significant hurdles, including problematic network latency, critical data privacy vulnerabilities, and a growing phenomenon of “technical fatigue” among frontline staff. This article explores the transition toward On-Device Edge AI—a paradigm where data processing occurs directly on the Neural Processing Units (NPUs) of handheld clinical hardware. By decentralizing intelligence and placing it directly at the point of care, hospitals can provide nurses with “Invisible Assistants” capable of ambient documentation, real-time policy guidance, and high-fidelity predictive alerting. This paper provides a comprehensive analysis of the implications for clinical efficiency, the quantifiable fiscal Return on Investment (ROI) for administrators, and the long-term mitigation of institutional liability and cybersecurity risks in an increasingly digital landscape.
Introduction: The Data Paradox in Modern Nursing
The contemporary nursing environment is defined by a striking “data paradox”: while hospitals collect a higher volume of patient data than at any point in history, the cognitive burden of managing, interpreting, and documenting this information has led to an era of significant professional strain. Nurses find themselves increasingly “tethered to the terminal,” spending a disproportionate amount of their 12-hour shifts navigating complex Electronic Health Record (EHR) interfaces rather than engaging in direct patient advocacy and care. This “digital desk work” is not merely an administrative nuisance; it is a primary driver of the nursing shortage, as clinicians feel disconnected from the human-centric mission that led them to the profession.
Traditional AI solutions designed to alleviate this burden have historically relied on cloud computing architecture. In this model, sensitive clinical data—ranging from voice recordings to high-resolution medical imagery—is transmitted over the hospital’s Wi-Fi to remote servers for processing. This centralized model is frequently compromised by the physical realities of the hospital environment: “dead zones” within lead-lined radiology suites, signal interference in elevators, and the inherent security risks of data-in-transit.
On-device Edge AI represents a fundamental shift in healthcare informatics by moving the “logic” of the AI from the cloud to the hardware itself. By utilizing specialized AI-accelerated chips (NPUs) integrated directly into ruggedized clinical handhelds, intelligence becomes localized and resilient. This ensures that the “brain” of the AI resides within the device in the nurse’s hand, allowing for instantaneous, offline, and private clinical support that operates with total independence from the hospital’s broader network fluctuations or external server downtimes.
Enhancing Clinical Efficiency: The “Invisible Assistant”
For the staff nurse, the primary value of Edge AI lies in the radical reduction of “scut work”—the repetitive, non-clinical administrative tasks that currently consume between 35% and 45% of a typical nursing shift. The goal is to move technology into the background, creating an “Ambient Intelligence” environment.
Ambient Documentation and the End of the “After-Shift” Charting
Retrospective charting remains one of the most significant stressors in the nursing workflow. It is common for nurses to spend an hour or more after their shift has officially ended to ensure that the EHR accurately reflects the day’s interventions. Edge AI facilitates “Ambient Documentation” through local Natural Language Processing (NLP). As a nurse performs a dressing change or conducts a patient assessment, the device’s NPU can listen to the verbal descriptions provided by the nurse, transcribe them in real-time, and automatically structure that data into the appropriate fields within the EHR.
Crucially, the on-device model provides a “Privacy-by-Design” solution that cloud-based competitors cannot match. In a cloud model, audio of a patient’s room might be streamed to an external server, raising immense HIPAA concerns. In the Edge AI model, the NPU converts the audio into structured text locally and immediately purges the raw audio file from the device’s memory. No voice recording ever leaves the room; only the finalized clinical data is synced. This eliminates the risk of intercepted audio and ensures that patient dignity is preserved while removing the latency associated with remote processing (MDPI, 2025).
The “Clinical Concierge”: On-Demand Policy and Formulary Chatbots
Information retrieval is a pervasive bottleneck in clinical settings. Nursing protocols are living documents, frequently updated to reflect new evidence-based practices. When a nurse needs to verify a specific facility-specific policy—such as the exact titration steps for a high-risk medication or the local protocol for a massive transfusion—they often must leave the bedside to find an open terminal and search the hospital intranet.
On-device Edge AI enables the deployment of “Clinical Chatbots” that are essentially localized Large Language Models (LLMs) trained exclusively on the institution’s internal manuals. A nurse can query their handheld: “What are the specific isolation requirements for a suspected C. diff patient on this floor?” or “What is the facility policy for needle-stick injuries?” The response is not a generic internet search but a precise, facility-sanctioned protocol delivered in milliseconds. Because these models are stored locally, they remain functional during network outages, ensuring that the nurse is never forced to rely on memory during a high-stakes clinical event.
The “Offline Advantage”: Clinical Resilience in Any Environment
The architectural resilience of Edge AI cannot be overstated. Standard hospital Wi-Fi is rarely uniform; elevators, basements, and stairwells often present connectivity gaps. In a traditional cloud-AI setup, a medication scan or a voice-to-text note would fail the moment the nurse stepped into a weak signal area, leading to data loss or workflow interruption. On-device AI ensures that med-scanning, diagnostic imaging support, and charting remain 100% available regardless of signal strength. This allows for a continuous flow of care, preventing the “digital friction” that contributes to nurse frustration and technical fatigue.
Administrative Implications: ROI, Throughput, and Risk Mitigation
From an administrative perspective, the adoption of Edge AI is a strategic financial imperative that addresses the core drivers of hospital operational costs and institutional risk.
Return on Investment (ROI) through Capacity Creation
In the current labor market, “Capacity Creation” is the most vital metric for hospital leadership. ROI is no longer just about the initial cost of a smartphone; it is about the “recovered clinical hours” of the existing workforce. Recent clinical informatics frameworks suggest that if Edge AI can save just 60 minutes of administrative burden per nurse per shift, a 500-bed facility effectively gains the equivalent of 25 to 30 additional full-time employees (FTEs) without a single new hire (Zetterström, 2024).
This recovered capacity directly drives:
Liability and Data Security: The “Closed-Loop” Security Model
The average cost of a healthcare data breach has risen to over $10.9 million, with “data-in-transit” being a primary vulnerability. By adopting an “Edge-First” approach, institutions fundamentally change their security posture. Since the “thinking” happens on the device, there is a drastic reduction in the amount of sensitive data being sent over the network. This “Closed-Loop” model makes it significantly harder for hackers to intercept sensitive patient data.
Furthermore, Edge AI acts as a robust “digital witness” during litigation. In the event of a sentinel event or an adverse outcome, administrators can access a millisecond-accurate “Clinical Audit Trail.” Unlike manual logs, which are often subject to human error or late entries, the Edge AI log provides an objective, tamper-proof record of exactly when a patient’s oxygen levels began to trend downward, when the AI-triggered alert reached the nurse’s handheld, and the exact moment the nurse acknowledged the alert. This level of granularity is essential in proving that the institution met the standard of care.
Rapidly Deployable Hardware and the Future of the Bedside
Edge AI is not a futuristic concept; it is a current reality. The hardware ecosystem required for this shift is already in production and ready for hospital-wide deployment.
Conclusion: Restoring the Human Element of Nursing
The integration of On-device Edge AI offers a rare opportunity to align the often-divergent interests of frontline clinicians and hospital leadership. For the nurse, it provides a tool that actively reduces cognitive load, protects professional autonomy, and restores the focus to the human-to-human connection of nursing. For the administrator, it provides a verifiable path to ROI through operational efficiency, staffing stability, and a robust defense against cybersecurity and legal liabilities.
As the healthcare landscape continues to evolve under the pressures of rising patient acuity and a shrinking labor pool, the institutions that succeed will be those that move beyond the “cloud” and empower their staff with intelligence that lives at the “Edge” of care. The future of nursing is not about navigating more screens; it is about utilizing invisible, local, and resilient technology to return the nurse to the patient’s side, where they are needed most.
References
American Hospital Association (AHA). (2025). Hospital Statistics and AI Integration Trends 2024-2025. AHA Research Group.
MDPI Qualitative Study. (2025). Perspectives on AI aiding decision-making and reducing physical exertion in care practices. Journal of Clinical Nursing and Informatics, 14(2), 112-128.
National Academy of Medicine. (2024). Artificial Intelligence in Health Care: The Hope, the Hype, and the Path Forward. National Academies Press.
Thompson, R., Lee, K., & Chen, M. (2023). AI-powered clinical decision support systems: Enhancing real-time evidence-based care. Healthcare Technology Review, 9(4), 45-59.
Zetterström, A. (2024). A framework for ROI in healthcare AI: Prioritizing administrative and edge-based efficiency. International Journal of Medical Management, 31(1), 12-24.

Author: Jude Chartier RN / AI Nurse Hub Date: March 30, 2026

By: Jude Chartier RN / AI Nurse Hub Date: March 23, 2026

By: Jude Chartier RN / AI Nurse Hub Date: March 19, 2026